Abstract
Background: Idiopathic pulmonary fibrosis (IPF) is a serious disease with a high mortality rate. Activation of transforming growth factor (TGF)-β1 production and signalling are considered the cornerstone in the epithelial-mesenchymal transition (EMT) process. EMT plays a central role in the development of fibrosis in many organs including the lungs. Activated platelets are an important source of TGF-β1 and play a pivotal role in EMT and fibrosis process. The antiplatelet, ticagrelor was previously found to inhibit the EMT in different types of cancer cells, but its ability to serve as an anti-pulmonary fibrosis (PF) agent was not previously investigated.
Objective: In this study, we aim to investigate the potential ability of ticagrelor to ameliorate bleomycin-induced fibrosis in rats.
Methods: PF was induced in rats by intratracheal BLM at a dose of 3 mg/kg. The effect of daily 20 mg/kg oral ticagrelor on different histological and biochemical parameters of fibrosis was investigated
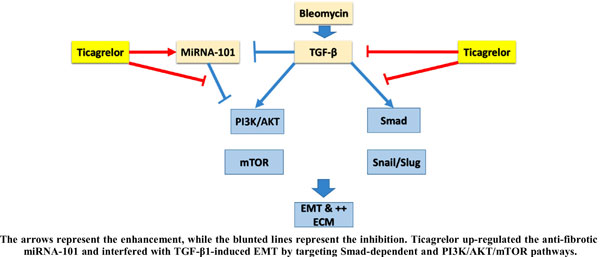
Results: Our results revealed that ticagrelor can alleviate lung fibrosis. We found that ticagrelor inhibited TGF-β1 production and suppressed Smad3 activation and signaling pathway with subsequent inhibition of Slug and Snail. In addition, ticagrelor antagonized PI3K/AKT/mTOR pathway signaling. Moreover, ticagrelor inhibited the EMT that was revealed by its ability to up-regulate the epithelial markers as E-cadherin (E-cad) and to decrease the expression of the mesenchymal markers as vimentin (VIM) and alpha-smooth muscle actin (α-SMA).
Conclusion: Our results suggest that the P2Y12 inhibitor, ticagrelor may have a therapeutic potential in reducing the progression of PF.
Keywords: Lung fibrosis, ticagrelor, bleomycin, TGF-β1, epithelial-mesenchymal transition, platelets.
[http://dx.doi.org/10.1084/jem.20110551] [PMID: 21727191]
[http://dx.doi.org/10.1073/pnas.0801414105] [PMID: 18641127]
[http://dx.doi.org/10.1136/annrheumdis-2013-203706] [PMID: 23852693]
[http://dx.doi.org/10.1016/S0002-9440(10)62351-6] [PMID: 15855634]
[http://dx.doi.org/10.1073/pnas.0804280105] [PMID: 18753630]
[http://dx.doi.org/10.1016/S2213-2600(17)30394-6] [PMID: 29066087]
[http://dx.doi.org/10.1186/rr36] [PMID: 11686863]
[http://dx.doi.org/10.1513/pats.200512-131TK] [PMID: 16738192]
[http://dx.doi.org/10.1097/MAJ.0b013e31821a9d8e] [PMID: 21613930]
[http://dx.doi.org/10.1186/1755-1536-3-2] [PMID: 20051102]
[PMID: 17645776]
[http://dx.doi.org/10.1038/srep35696] [PMID: 27774992]
[http://dx.doi.org/10.1083/jcb.200611146] [PMID: 17646396]
[http://dx.doi.org/10.1016/j.ccr.2011.09.009] [PMID: 22094253]
[http://dx.doi.org/10.1182/blood-2012-06-438598] [PMID: 22966171]
[http://dx.doi.org/10.18632/oncotarget.8655] [PMID: 27074574]
[http://dx.doi.org/10.1124/mol.113.084988] [PMID: 23580446]
[http://dx.doi.org/10.1182/blood-2017-02-769893] [PMID: 28679740]
[http://dx.doi.org/10.1007/s10555-018-9730-4] [PMID: 29855749]
[PMID: 24889539]
[PMID: 26483688]
[http://dx.doi.org/10.1136/jcp.41.4.467] [PMID: 3366935]
[http://dx.doi.org/10.1007/s00441-018-2879-x] [PMID: 29987390]
[http://dx.doi.org/10.3892/mmr.2011.425] [PMID: 21468558]
[http://dx.doi.org/10.1016/j.matbio.2018.02.007] [PMID: 29428229]
[http://dx.doi.org/10.1074/jbc.M117.805747] [PMID: 28726637]
[PMID: 29186838]
[http://dx.doi.org/10.1007/s13402-015-0247-3] [PMID: 26458815]
[http://dx.doi.org/10.1016/S0021-9258(18)32345-7] [PMID: 6602130]
[http://dx.doi.org/10.1074/jbc.274.43.31008] [PMID: 10521498]
[PMID: 21135509]
[http://dx.doi.org/10.1007/s11926-019-0815-z] [PMID: 30830444]
[PMID: 25959210]
[PMID: 26289670]
[http://dx.doi.org/10.1038/s41591-018-0087-6] [PMID: 29967351]
[http://dx.doi.org/10.1016/S0140-6736(17)30866-8] [PMID: 28365056]
[http://dx.doi.org/10.1016/j.ajpath.2012.02.004] [PMID: 22387320]
[http://dx.doi.org/10.1002/ijc.20945] [PMID: 15729716]
[PMID: 12370004]
[http://dx.doi.org/10.1002/ijc.28947] [PMID: 24798403]
[PMID: 29322294]
[PMID: 27929137]
[PMID: 29958560]
[http://dx.doi.org/10.1371/journal.pone.0070725] [PMID: 23967091]